Summary
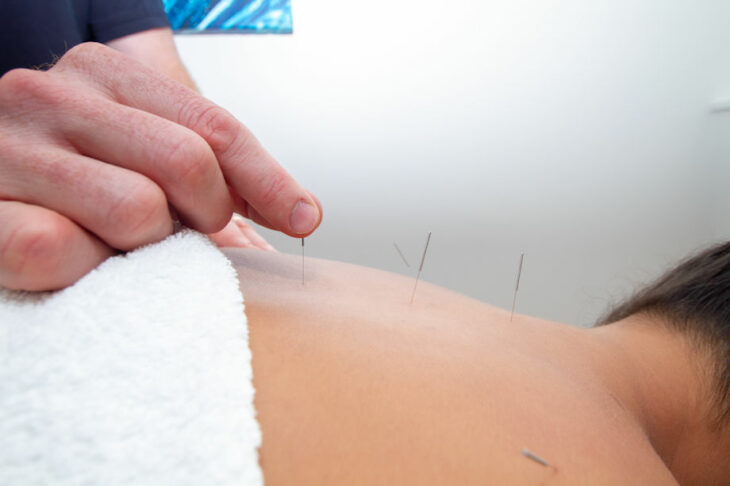
Back pain affects millions of people worldwide, but surgery and medication aren’t your only options. Acupuncture is a science-based treatment that activates your nervous system’s natural pain-relief mechanisms, improving blood flow and promoting healing without the side effects of pharmaceuticals. We integrate Acupuncture with complementary therapies to address the root causes of your back pain and restore your quality of life.

Why Back Pain Persists
Back pain is one of the most common health complaints globally, affecting people across all ages and lifestyles. Whether from desk work, sports injuries, or simply the wear and tear of daily life, persistent back pain can be debilitating. The problem is that conventional treatments often focus on symptom management rather than addressing underlying causes.
Most people reach for over-the-counter pain relievers or are prescribed stronger medications, but these come with significant risks. Long-term, high-dose NSAID use has been linked to a greater risk for heart attack, stroke, heart failure and death from cardiovascular disease. Studies published in The Lancet (based on data from 639 randomised trials involving over 300,000 people) show that heart attack and stroke risk increase even with short-term NSAID use, and the risk may begin within a few weeks of starting to take an NSAID. Research from the Agency for Healthcare Research and Quality found that opioids are associated with small improvements versus placebo in pain and function at short-term follow-up, with evidence of increased risk of serious harms that appear to be dose dependent.
Surgery is often presented as the next option, yet most back pain improves naturally over time or with self-care. The question becomes: how do we accelerate healing and reduce pain safely?
The Science Behind Acupuncture for Back Pain
Acupuncture is far more than ancient tradition. When we place needles at specific points on your body, we’re stimulating your nervous system in precise, measurable ways.
How Acupuncture Works at the Biochemical Level:
When Acupuncture needles stimulate specific points, they trigger your body to release endorphins (your natural painkillers) and activate the parasympathetic nervous system (your “rest and repair” mode). This shift is crucial because chronic stress keeps your nervous system in “fight or flight,” which amplifies pain perception and delays healing.
Additionally, Acupuncture stimulates the release of neurotransmitters like serotonin and dopamine, which regulate pain signals in your brain. The treatment also increases blood flow to affected tissues, improving oxygen and nutrient delivery essential for healing damaged muscle and connective tissue.
At the cellular level, Acupuncture regulates adenosine (involved in pain reduction and tissue healing) and ATP (the energy molecule your cells need for repair). These aren’t metaphorical changes they’re measurable biochemical shifts that accelerate your body’s natural healing capacity.
Why Back Pain Particularly Responds to Acupuncture:
Your back contains multiple layers of muscles, nerves, and connective tissues. Back pain often stems from muscular tension, nerve irritation, or postural imbalance rather than structural damage. Acupuncture addresses these soft-tissue issues by releasing myofascial tension and improving local circulation without the inflammation that medications can cause.
The Three Types of Back Pain and How Acupuncture Helps
Upper Back Pain
Upper back pain often results from poor posture, desk work, or stress-related tension. The thoracic spine (your upper back’s 12 vertebrae) connects your head to your hips while protecting vital organs like your lungs and heart.
Acupuncture for upper back pain targets points that release tension in the neck, shoulders, and between the shoulder blades. By calming your nervous system, Acupuncture reduces the stress-driven muscle tension that perpetuates upper back pain.
Lower Back Pain
The lumbar spine (your lower back’s 5 vertebrae) bears the weight of your entire torso and head. It’s the most common site of back pain because it absorbs tremendous force daily.
Lower back pain often involves nerve irritation or muscular guarding (protective muscle tension). Acupuncture stimulates pressure points in the lower back, feet, knees, and hips to release this guarding pattern and restore proper nerve function.
Chronic vs. Acute Back Pain
Acute back pain (recent injury) responds quickly to Acupuncture because inflammation and muscular tension are the primary issues. Chronic back pain (lasting months or years) requires a longer treatment course because your nervous system has learned to perceive pain even after the original injury heals. Acupuncture retrains your nervous system, gradually decreasing pain signals.
What to Expect During Your First Acupuncture Session
Understanding what happens during treatment removes anxiety and helps you experience maximum benefit.
The Assessment:
We begin by asking detailed questions: When did your back pain start? What activities aggravate or improve it? Do you sleep well? We may request diagnostic imaging (X-ray, ultrasound) to identify structural issues, though many back conditions don’t show on imaging even though they cause significant pain.
The Treatment:
During your session, you’ll lie face-down on a comfortable treatment table while we insert thin, sterile needles at specific points. The needles are so fine that insertion is usually painless. Once needles are positioned, we leave you to relax for 30 to 45 minutes as your nervous system responds.
You’ll likely experience a profound sense of relaxation during treatment. Many patients report mild euphoria, deep relaxation, or simply a sense of calm. This is your parasympathetic nervous system activating your body’s healing capacity.
Post-Treatment Care:
After treatment, we recommend light hydration, rest, and avoiding strenuous activity for 24 hours. Your body enters an active healing phase, and rest optimises this process. You may experience temporary mild soreness or fatigue this is normal and indicates your nervous system is rebalancing.
Realistic Outcomes and Treatment Frequency
Most patients experience some pain relief after the first session. However, lasting relief typically requires consistent treatment over several weeks.
For acute back pain (recent injury), we typically recommend 6 to 12 sessions over 2 to 3 months. For chronic back pain (months or years of symptoms), we recommend 12 to 20 sessions over 2 to 3 months, then ongoing maintenance sessions monthly or as needed.
The frequency matters because your nervous system needs repeated stimulation to learn new pain pathways. Think of it like physical rehabilitation: one visit to the gym doesn’t build strength, but consistent training does.
Many patients discover that their pain doesn’t return completely to previous levels once treatment concludes. You’ve essentially retrained your nervous system to perceive less pain and your tissues have healed more completely.
Why We Avoid Over-Reliance on Medications
Our philosophy is simple: treatments should work with your body, not replace its natural healing capacity.
OTC pain relievers provide temporary relief but mask underlying issues and carry cardiovascular risks. Muscle relaxants cause drowsiness and don’t address root causes. Even Cortisone injections provide only temporary relief (usually less than a few months) and repeated injections can damage surrounding tissue.
Acupuncture is different. It stimulates your body’s own healing mechanisms. Over time, your nervous system becomes more resilient, pain sensitivity decreases, and your tissues heal more completely.
Ready to Address Your Back Pain?
Back pain doesn’t have to be a lifelong condition. Whether your pain is from a recent injury, chronic muscular tension, or postural imbalance, we have the science-based tools to help you heal.
We combine Acupuncture with Remedial Massage, Cupping Therapy, Heat Therapy, and personalised exercise guidance to address your unique situation. Our integrated approach targets both the nervous system and muscular components of your pain.

Book your personalised assessment online or call us on (02) 4709 6727. We look forward to discussing how we can help you achieve lasting back pain relief and reclaim your quality of life.