Quick Summary
Headache disorders are common neurological conditions affecting many people worldwide, regardless of age, race, or gender. They include tension-type headaches, migraines, cluster headaches, and medication-overuse headaches. These conditions can cause symptoms such as nausea, insomnia, and severe pain. Almost half of the adult population experiences a headache at least once a year. Treatment varies from medications and personal preventative measures to alternative therapies like acupuncture and massage. Understanding triggers and managing lifestyle factors can also help prevent headaches.
What Are Headache Disorders?
Headache disorders are among the most common disorders of the nervous system. They can affect anyone regardless of age, race, and gender. The pain of headaches can occur in any region of the neck and head, although the symptoms that arise due to headaches can be worse, such as nausea and insomnia.
Did you know, almost half of the adult population have had a headache at least once within the last year? Headaches are underestimated, under-recognised and under-treated throughout the world.
What Are The Different Types Of Headaches?
Headache disorders are categorised into four types with the following symptoms:
1. Tension-Type Headache (TTH)
Tension-type headaches are the most common type of headache. It is described as pressure or tightness, often like a band around the head, sometimes even spreading to the neck and shoulders. The pain can last from 30 minutes to several days or maybe continuous. The most common causes of TTH are anxiety, emotional stress, depression, poor posture, eye strain and lack of sleep.
Signs and symptoms of a tension headache include:
- Dull and painful head pain.
- The sensation of tightness or pressure across your forehead, side and back of the head.
- Tenderness over the scalp, neck and shoulder regions.
2. Migraine
Many people who experience migraines feel unwell for a short period beforehand. Some people see flashing lights, change in their vision or have problems speaking. This is what they call an ‘aura’ and typically happens before the headache starts. When the headache starts, it is usually severe. Your heads throb and it might hurt to see bright lights or hear noises. You might feel sick and like you need to vomit. This can last anywhere between a few hours and a few days.
Studies have shown that migraines affect over 3 million Australians and are twice as common in women due to hormonal factors. Migraines often begin at puberty, but often it appears in an individual in their 20s or 30s. It can also be due to genetics.
A migraine headache is caused by abnormal brain activity, which can be triggered by many things including hormonal changes, emotional triggers, medications or physical causes such as insomnia. The exact cause remains unclear though. Most medical experts believe the attack begins in the brain and involves nerve pathways and chemicals. The changes affect the way nerves communicate as well as affecting blood flow in the brain and surrounding tissues.
3. Cluster Headache (CH)
A cluster headache starts and ends suddenly, it strikes quickly, usually without warning. Although cluster headaches are short, they are extremely painful and can occur every day for weeks or months at a time. The cause of cluster headaches is unknown but does involve a nerve in the face, which creates intense pain around the eyes. Cluster headaches can be more severe than a migraine, although they usually don’t last as long.
Physical symptoms of a cluster headache include:
- Swollen, teary and red eyes
- Runny or blocked nose
- Red, warm face
- Being sensitive to light
- Discomfort or a mild burning sensation in the face
4. Medication-Overuse Headache (MOH)
People who use acute pain-relief medicine such as Panadol or codeine more than ten days out of the month can set off a cycle called ‘medication-overuse headaches’ (MOH). As the medicine wears off, the pain comes back which then influences the individual to take more. Over time the medicine stops being helpful and starts to become harmful, which then causes headaches. This can occur whether the individual was taking medicine for headaches in the first place or for another type of pain/condition. MOH can occur with both over the counter and prescription pain-relief medicines.
Signs symptoms of medication-overuse headaches:
- Occur nearly every day which often wake you up early in the morning – restlessness
- Improve with pain relief medication but then return as your medication wears off
- Nausea
- Difficulty concentrating or retaining information
- Irritability

Causes Of Headache Disorders
There are many factors which can lead to headaches or migraines.
Therefore, the importance of diagnosing and treating the correct cause is important.
Headaches or migraines might be caused by:
- Muscular tension
- Inflammation
- High blood pressure
- Low blood pressure
- Malnutrition/Diet
- Blood-borne toxins due to organ dysfunction or injury
- Decreased blood circulation due to injuries
- Insomnia
- Emotional stressors
- Hormonal disturbances
- Medication overuse
Treatment Of Headache Disorders
There are a variety of ways to help assist in reducing and eliminating headaches. Treatments available consist of:
- Medications
- Personal preventative measures
- Acupuncture
- Massage
Medications
The main medication used to treat headache disorders include:
- Pain reliefs (aspirin, paracetamol, ibuprofen)
- Anti-emetics – specific anti-migraine medications
In addition to this, practitioners of herbal medicine use various formulations of naturally occurring herbs to treat headache disorders.
When considering pharmaceutical medication to treat headache disorders, it is important to note that headaches may also be caused by misuse of aspirin and other ‘pain killers’. Other common side effects of these types of medication include gastrointestinal bleeding, stomach ulcers, stroke and heart attack.
Personal Preventative Measures
Knowing your trigger for headaches enables you to start your headache prevention program. An idea to help get to the bottom of why you are frequently having headaches is to write down in a diary what you are eating, drinking and doing in a day. By doing this, you can look back and see what you are doing wrong and play the elimination game to find the cause. The most common ways to avoid stress are as follows;
- Avoid alcohol or smoking
- Get an appropriate amount of sleep
- Limit your caffeine intake
- Exercise
- Eat a well-balanced diet and drink more water
- Manage stress by finding a hobby
- Maintain good posture, and move around during the day
Chinese Herbal Medicines
If you’re looking for a more safe, natural and chemical-free treatment to improve headache/migraines, Chinese Herbal Medication is the way to go. To achieve the best possible outcomes and avoid side effects, herbal medications are made up in formulations of anywhere from 2-30 different herbal medications.
Herbal medicine practitioners prepare unique formulations of herbal medicine to best suit the individual and their specific needs.
Acupuncture
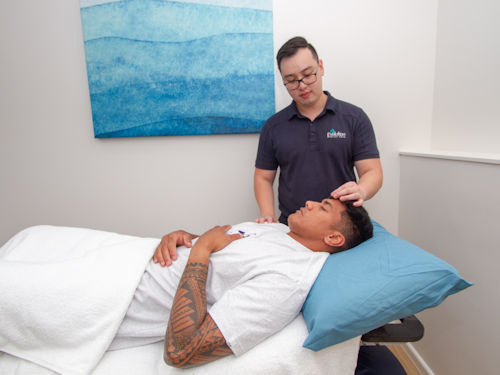
There has been significant research conducted on this innovative medical treatment about headache disorders.
There is currently strong evidence supporting the effectiveness of acupuncture for the treatment of Headache disorders and Migraine.
Acupuncture appears to improve quality of life for many chronic headache and migraine sufferers at a relatively low cost when compared to alternatives.
Acupuncture is considered safe with a low incidence of minor adverse effects when performed by a qualified practitioner and there is no other non-drug therapy that works better for pain reduction.
Acupuncture seeks to restore the flow of positive energy throughout your body as well as removing negative energy. Acupuncture needles are inserted into different positions in the body, usually close to nerves. The positioning of needles depends on the symptoms the individual is experiencing. The needles stimulate the nerves to release endorphins. The endorphins, also known as the ‘feel good’ chemicals, are then released throughout your body, as well as stimulating the immune and circulation system in your body which relieves the headaches.
Massage
Massages are a great way to reduce stress and relieve tension. Muscle tension can be the cause of headaches for some individuals. Massages help with the tightness of muscles in the back of the head, neck, and shoulders. Research shows that massages can decrease pain, tension, duration, intensity, and frequency of headaches.